Regenerative medicine is changing the game in orthopedics. Instead of just managing pain or symptoms, regenerative solutions aim to restore the structure and function of damaged tissues, offering long-term solutions for conditions like cartilage lesions, tendon tears, and bone defects.
This approach leverages the body’s own healing power, supported by advanced technologies such as biologic scaffolds, stem cells, or platelet-rich plasma (PRP) to stimulate tissue regeneration. Our proprietary Hyaff® technology takes hyaluronic acid (HA), a natural component of healthy tissue, and transforms it into a biocompatible scaffold that creates a favorable environment for cell growth and tissue regeneration.
This is especially valuable in orthopedics, where cartilage, tendon, and bone have limited natural healing capacity due to low blood flow and other factors.1
Cartilage Repair
Cartilage damage is difficult to treat due to its avascular nature, meaning there are very few blood vessels or a lack of blood supply found, which limits the tissue’s intrinsic healing capacity.14 Orthopedic regenerative medicine approaches have emerged as promising solutions for various joint conditions. These regenerative solutions aim to restore functional hyaline-like cartilage rather than scar-like fibrocartilage and offer alternatives through advanced techniques such as our hyaluronic acid scaffold, Hyalofast®. Hyalofast is a single-stage, off-the-shelf 3D matrix made from our proprietary Hyaff (esterified hyaluronic acid) technology. It facilitates the adhesion and entrapment of cells in the injury site, supporting their multi-dimensional development (i.e. cell migration and proliferation) and creating an HA-rich environment that promotes the differentiation and proliferation of the cells, inducing cartilage regeneration.12,13 HA promotes repair by guiding cells through these critical steps of tissue healing.
Ultimately, regenerative solutions like Hyalofast aim to regenerate hyaline-like cartilage, improve joint function, delay or prevent osteoarthritis progression, and significantly reduce pain.2

Tendon Repair
Tendons are highly susceptible to injury and degeneration due to repetitive stress, overuse, and the natural aging process. These injuries commonly affect athletes and active or aging individuals and are often difficult to treat because tendons have limited blood supply and a reduced capacity for self-repair.5 Some treatments, such as rest, physical therapy, or surgery can help, but they may not fully restore tendon strength or function. That’s where orthopedic regenerative medicine comes in. Regenerative approaches can include our highly differentiated HA-based implant, Integrity™, PRP (or Platelet-Rich Plasma) injections or collagen scaffolds. The Integrity Implant is a hyaluronic acid-based scaffold that is reshaping tendon repair by engaging the body’s natural, biologic healing processes. Integrity is specifically engineered to support tendon healing by combining the high strength of a knitted polyester mesh with the therapeutic benefits of hyaluronic acid, which helps regulate inflammation and creates an optimal environment for tissue remodeling and regeneration.7-9
Distinctive regenerative solutions like Integrity are designed to foster healing, improve tissue quality, and help patients return to the activities they love with greater confidence.
We strongly believe Hyaff is the best way to treat cartilage and tendon repair.
Bone Regeneration
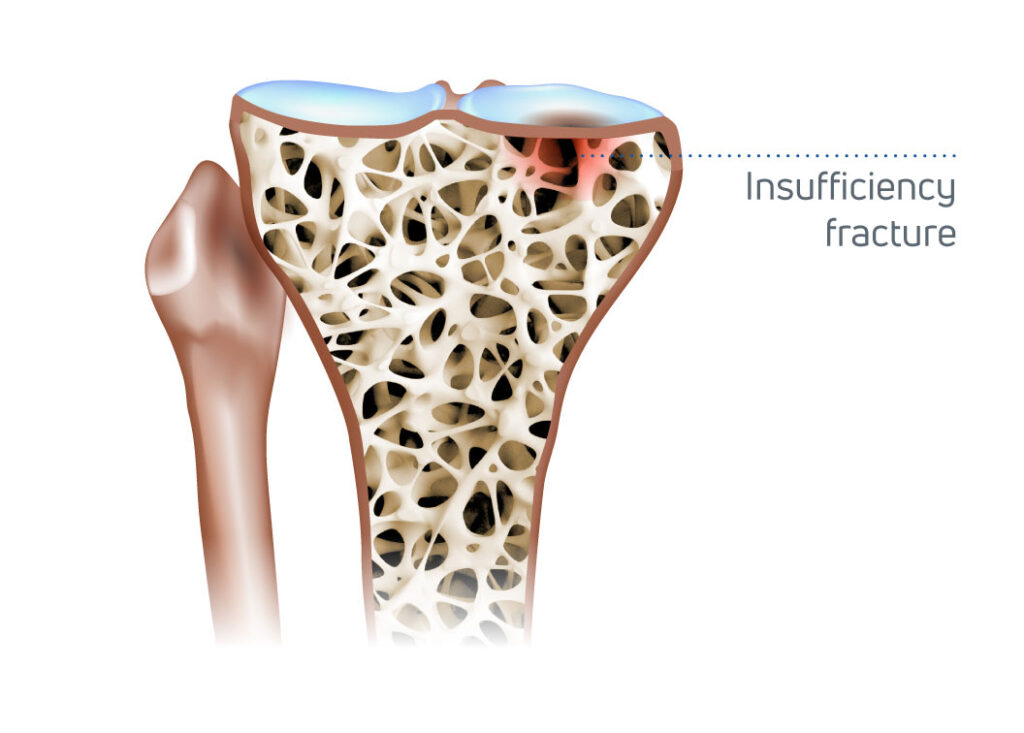
Bone defects and fractures that fail to heal properly can pose significant challenges for patients and physicians. These conditions may arise from trauma, osteoporosis, or compromised blood supply, and they can lead to long recovery times, pain, and loss of mobility.11 Bone defects, or insufficiency fractures (small cracks in the bone), can benefit from regenerative approaches such as Tactoset®, our innovative HA-enhanced injectable bone substitute, or from other approaches including bone cements, grafts, or fillers. Tactoset is a minimally invasive solution that can help restore stability and promote new bone growth (osteogenesis) allowing people to resume their daily activities with reduced pain.2
The Role of Hyaluronic Acid in Regenerative Medicine
Hyaluronic acid (HA) is naturally occurring and found throughout the body, particularly within the extracellular matrix of connective tissues and joint structures. Its unique physical and biocompatible properties make it an ideal biomaterial for regenerative applications.
We modify HA through our proprietary esterification process to enhance its stability and mechanical strength. Our Hyaff (HA) scaffolds are used to guide tissue regeneration, supporting natural healing.3
Biocompatibility and biodegradability
HA is well tolerated by the body and breaks down into natural, non-toxic components when implanted or injected.
Hydration and viscoelasticity
Its ability to retain water and provide cushioning makes it essential in joint lubrication
Cell signaling and scaffold support
HA interacts with cell surface receptors like CD44, influencing cell adhesion, proliferation (cell growth), and differentiation (specialized into the right type of tissue), creating the conditions needed for effective healing and regeneration.3
Regenerative medicine is reshaping orthopedic care by shifting the focus from symptom management to true biologic healing. Unlike traditional approaches that often rely on mechanical repair alone, regenerative strategies leverage the body’s own capacity for healing, aiming to restore native tissue function and durability by offering biologically driven, minimally invasive treatments that promote true healing.10 Hyaluronic acid stands out as an essential component in orthopedics, supporting the regeneration of cartilage, tendon, and bone through its unique properties and adaptability. As clinical research advances, HA-based technologies are expected to play an even greater role in personalized orthopedic care, offering biologically driven solutions that can improve long-term musculoskeletal health.
- Regenerative Medicine for Orthopedics: Biologic Therapies – HSS(opens in a new tab)
- Regenerative Medicine in Orthopaedic Surgery: Pioneering Advances and…(opens in a new tab)
- Hyaluronic acid: a versatile biomaterial in tissue engineering(opens in a new tab)
- The Role of Hyaluronic Acid in Tissue Engineering(opens in a new tab)
- Sharma P, Maffulli N. Biology of tendon injury: healing, modeling and remodeling. J Musculoskelet Neuronal Interact. 2005.
- Andia I, Maffulli N. Platelet-rich plasma for managing pain and inflammation in osteoarthritis. Nat Rev Rheumatol. 2013.
- Polizzi, A., et al. Impact of Hyaluronic Acid and Other Re-Epithelializing Agents in Periodontal Regeneration: A Molecular Perspective. Int. J. Mol. Sci. 2024, 25, 12347. https://doi.org/10.3390/ijms252212347(opens in a new tab)
- Chen WYJ, Abatangelo G. Functions of hyaluronan in wound repair. Wound Repair Regen. 1999.
- Anika Therapeutics. Data on file.
- Mao AS, Mooney DJ. Regenerative medicine: Current therapies and future directions. Proc Natl Acad Sci USA. 2015.
- Einhorn TA, Gerstenfeld LC. Fracture healing: mechanisms and interventions. Nat Rev Rheumatol. 2015 Jan;11(1):45-54. doi: 10.1038/nrrheum.2014.164. Epub 2014 Sep 30. PMID: 25266456; PMCID: PMC4464690.
- Kon, E., Filardo, G., Roffi, A., Andriolo, L., & Marcacci, M. (2012). New trends for knee cartilage regeneration: From cell-free scaffolds to mesenchymal stem cells. Current Reviews in Musculoskeletal Medicine, 5(3), 236–243. https://pmc.ncbi.nlm.nih.gov/articles/PMC3535079/(opens in a new tab)
- Gobbi A. One-Step Cartilage Repair of Full-Thickness Knee Chondral Lesions Using a Hyaluronic Acid-Based Scaffold Embedded With Bone Marrow Aspirate Concentrate: Long-term Outcomes After Mean Follow-up Duration of 14 Years. Am J Sports Med. 2024 Dec;52(14):3561-3568. Epub 2024 Nov 3. https://pubmed.ncbi.nlm.nih.gov/39491512(opens in a new tab)
- Mithoefer, K., McAdams, T., Williams, R. J., Kreuz, P. C., & Mandelbaum, B. R. (2009). Clinical efficacy of the microfracture technique for articular cartilage repair in the knee: An evidence-based systematic analysis. American Journal of Sports Medicine, 37(10), 2053–2063. https://doi.org/10.1177/0363546508328414(opens in a new tab)
